Faecal occult blood testing using FIT in suspected colorectal cancer
Resource
Faecal occult blood (FOB) is the detection of blood in the faeces which is not visually apparent. When colorectal cancer is present, the concentration of human haemoglobin detectable in faeces increases. NICE DG30 Quantitative faecal immunochemical tests to guide referral for colorectal cancer in primary care (July 2017) recommends faecal occult blood (FOB) testing in primary care patients to guide referral for suspected colorectal cancer in people without rectal bleeding who have unexplained symptoms but do not meet the criteria for a suspected cancer pathway referral detailed in NICE NG12 Suspected Cancer; recognition and referral.
Faecal immunochemical testing (FIT) is a more sensitive and specific method of detecting human haemoglobin than traditional chemical methods.
FOB should be used as a test to triage the most appropriate patients for colonoscopy, to try to target and detect cancer earlier and avoid unnecessary invasive investigation in those at low risk. Using FIT gives excellent negative predictive value for ruling out colorectal cancer, 99.8% with our method, using a cut-off of 10µg/g. NICE recommend patients in the following categories are offered FOB testing.
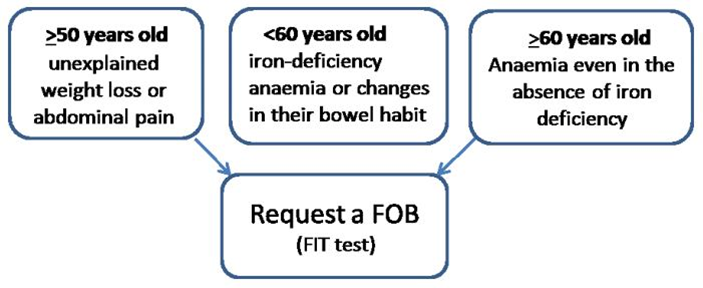
Referral should not be delayed by waiting for FOB results in patients with red flag symptoms who are at higher risk of colorectal cancer. NICE recommend patients in the following categories are urgently referred via the two week pathway.

FIT is available on ICE. If you need a FIT device and do not have one please use the contact numbers. Each device comes with an instruction leaflet detailing how the sample should be collected, labelled and delivered back to the GP surgery to be transported to Clinical Biochemistry. Results will be reported as Positive or Negative via ICE. We will use a cut-off of 10µg/g to determine if results are positive or negative, as recommended by NICE.
Please be aware that they are very different to current FOB kits.
The following algorithm is a locally agreed care pathway between Clinical Biochemistry, Gastroenterology and Endoscopy. This will provide safety-netting for patients with negative FOB results where clinical suspicion remains.
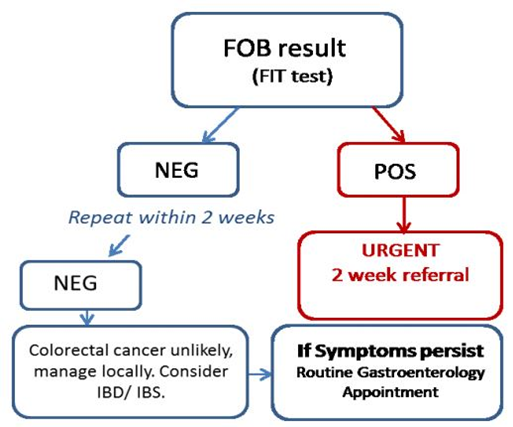
Please advise patients that even if they have had a recent national screening FOB test which was negative, once symptomatic, this test is valuable and may be positive (since different cut-offs are used for asymptomatic screening).
Website:
www.faecal-immunochemical-test.co.uk
Information video for primary care:
UHS clinical queries:
023 8077 7222 and ask for bleep 2612.
UHS re-ordering 023 8120 8717
HHFT clinical queries:
Michelle Young: 01256 313 270 michelle.young@hhft.nhs.uk
Kirsty Gordon: 01256 313 285 / kirsty.gordon@hhft.nhs.uk
HHFT re-ordering: pathology.supplies@hhft.nhs.uk

