Blog: Reducing antibiotic prescribing in WHCCG practices – A system-wide approach
News
Liz Corteville, Locality Lead Pharmacist, Medicines Optimisation Team, NHS West Hampshire Clinical Commissioning Group, has written a blog about improved antibiotic use in the local area.
International comparisons show that antibiotic resistance rates are strongly related to antibiotic use in primary care. So any national strategy to reduce antimicrobial resistance needs to target antibiotic prescribing in primary care. In the UK, around 80% of antibiotic prescribing occurs in the community. Although nationally antibiotic prescribing rates have fallen, studies show substantial overprescribing of antibiotics, particularly in uncomplicated respiratory tract infections.
In April 2018, WHCCG was 10% below the national (England) average antibiotic prescribing rate for total antibiotics but 35% above the national average for co-amoxiclav prescribing rates. This coupled with considerable inter- and intra-practice childhood antibiotic variation led to a WHCCG antimicrobial stewardship (AMS) campaign.
The WHCCG Medicines Optimisation Team (MOT) – consisting of clinical pharmacists and pharmacy technicians working in WHCCG practices – were trained in-house to deliver AMS educational outreach meetings, offered as part of a medicines optimisation incentive scheme and taken up by all 48 practices. Lead practice clinicians appointed as AMS champions prepared bespoke practice- and clinician-level antibiotic data and all practice staff were encouraged to attend the outreach meeting. The interactive workshop showcased resources from the Public Health England and Royal College of General Practitioners, such as the Treat Antibiotics Responsibly Guidance Education Tools (TARGET), an antibiotics toolkit, and the Healthier Together (HT) website.
Launched by Wessex Strategic Clinical Networks in April 2014, HT aims to improve the health of 0-18 year-olds in Hampshire, Dorset and the Isle of Wight. The programme was co-designed with parents and healthcare professionals from primary and secondary care. The strategy focused on healthcare professional and parental education and promoted shared decision-making. The HT website includes a parental SMS link and a comprehensive training programme was devised for all professional groups across the healthcare system, allowing delivery of consistent advice on the parent portal.
In the year following the educational outreach intervention, WHCCG mean antibiotic prescribing rate reductions were greater than the national average. Twelve-month rolling averages (per 1,000 patients) in September 2018 were compared to September 2019 for all three measures:
- Total oral antibiotic dispensed items fell by 9.4% (England equivalent 6.9%)
- Oral co-amoxiclav dispensed items fell by 15% (England equivalent 5%). WHCCG co-amoxiclav dispensing rates fell from 35% to 22% above the England average.
- Antibiotic dispensed items in 0-4 year-old children fell by 17% (England equivalent 6%).
Comparing items (per 1,000 patients) across WHCCG over a six-month winter period (October – March) 2018/19 to winter 2017/18:
- Total oral antibiotic dispensed items fell by 11% (England equivalent 8% )
- Oral co-amoxiclav dispensed items fell by 20% (England equivalent 8% )
- Antibiotic dispensed items in 0-4 year-old children fell by 19% (England equivalent 6%). The impact of this intervention was most significant in young children.
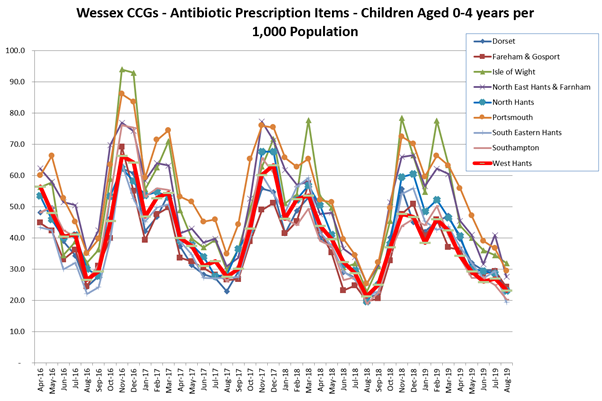
Graph above: variation in antibiotic prescribing in young children between CCGs in Wessex; 2016-2019 data
In contrast, antibiotic prescribing rates in elderly patients (over 75 years) who were not specifically targeted by the educational materials fell by a similar rate in WHCCG (5.4%) compared to England (4.5%) during the same time period.
In conclusion, by incentivising practices to undertake TARGET antibiotic workshops run by local facilitators and promoting the HT resources and approach, WHCCG improved antibiotic use, promoted responsible AMS and reduced unnecessary patient exposure to antibiotics and primary care workload associated with inappropriate antibiotic use. The impact of this intervention was most significant in young children.
